Thank you for your interest!
Help drive breakthroughs in ocular health by joining our research studies. Using state-of-the-art technology, we explore new treatments and deepen our understanding of ocular surface health.
Our research has contributed to advancements in therapies for dry eye, contact lenses, and related conditions. We conduct studies on:
- Dry eye
- Contact lens wear
- Tear collection
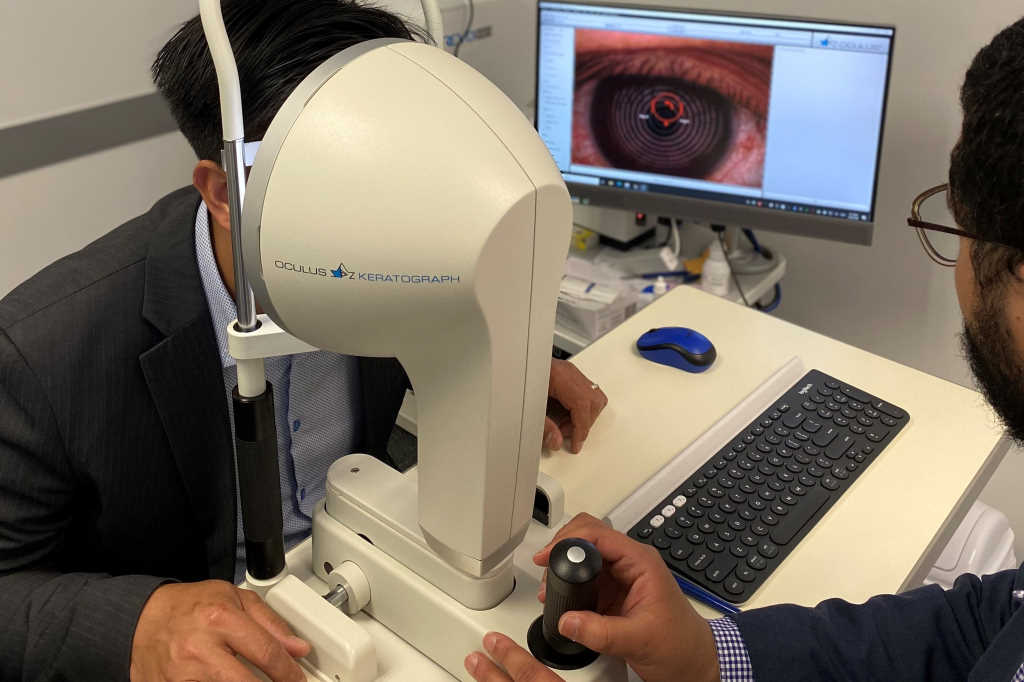
- Ocular surface imaging and analysis
- Epidemiology studies
Join our volunteer community today! Explore the categories below to learn about current studies seeking participants.
Understanding the role of inflammasomes
Doctoral Candidate, Dian Zhuang’s research focuses on understanding the role of inflammasomes, particularly NLRP3, and associated inflammatory markers such as Interleukin-1 beta (IL-1β) and IL-18 in dry eye disease (DED). DED is a common and often undertreated condition characterised by tear film instability, hyperosmolarity, and chronic inflammation of the ocular surface. Currently available anti-inflammatory treatments, such as corticosteroid eye drops, can offer temporary relief but are associated with considerable side effects, including cataract formation and raised intraocular pressure. Moreover, preservatives in many formulations can further exacerbate symptoms. Therefore, there is an urgent need for safer, more effective therapeutic options.
Dian’s study seeks to contribute to the growing understanding of DED, involving comparing the levels of inflammasome markers in the tears and conjunctival cells of both DED patients and healthy individuals. Inflammasomes have been reported to be significantly upregulated in the tears and ocular surface of DED patients [1,2]. By elucidating the role these markers play in the pathophysiology of DED, the research aims to inform the development of a novel preservative-free eye drop treatment, currently run in parallel by the BOTU team, that targets the underlying causes of the disease. This innovative approach may offer patients a safer alternative to current therapies and improve their overall quality of life.
The current study is still recruiting participants with moderate-severe dry eye. If you are interested, please click the link for participation: Exploring inflammation in dry eye disease – The University of Auckland
Reference:
[1] Niu L, Zhang S, Wu J, Chen L, Wang Y. Upregulation of NLRP3 inflammasome in the tears and ocular surface of dry eye patients. PLoS One 2015;10:e0126277. https://doi.org/10.1371/journal.pone.0126277.
[2] Zhuang D, Misra SL, Mugisho OO, Rupenthal ID, Craig JP. NPRL3 inflammasome as a potential therapeutic target in dry eye disease. Int J Mol Sci 2023;24:1–20. https://doi.org/10.1016/j.survophthal.2021.04.006.
Squeezability of eye drop bottles
As people age or suffer from arthritis, their risk for chronic eye conditions like dry eye disease and glaucoma increases, often requiring ongoing treatment with eye drops. However, self-administering these drops can be surprisingly challenging.
New preservative-free delivery systems, such as single-use minims and eye sprays, aim to reduce side effects but introduce additional complexities. Tasks like twisting off lids and precise aiming require good grip and pinch strength, which can be limited in the elderly and those with arthritis.
This project seeks to evaluate the difficulties faced by elderly when using non-traditional eye drop delivery methods. We will explore the relationship between grip strength and the challenges of self-instillation, aiming to identify ways to enhance patient support and improve ocular health management.
“Are you 65 years and older and have arthritis? Do you have trouble using eye-drop bottles? Participants are needed for an Auckland-based study! For more information, please contact: Kalika Bandamwar, Research Fellow, The Ocular Surface Laboratory, Department of Ophthalmology, Faculty of Medical and Health Sciences, University of Auckland. Phone number: 022 393 7246 (022 EYE PAIN) and Email address: kalika.bandamwar@auckland.ac.nz