Knowledge Centre
Stay informed on the latest research from the Ocular Surface Lab DRY EYE ASSOCIATIONPUBLICATIONSExplore the latest scientific research and evidence-based innovations shaping clinical decision-making for dry eye care.
Our curated compendium features:
- Patient resources, including educational videos and practical tips
- Summaries of key scientific studies
- Insights into future possibilities
Focused on clinical applications, these resources provide valuable guidance for improving dry eye management in practice.
Patient Videos and Tips
Research Highlights
Understanding Dry Eye: A Common but Complex Condition
Dry eye can be one of the most life-disrupting chronic eye problems. This is why a thorough examination is essential to uncover the root cause and ensure the right treatment is provided.
The term “dry eye” refers to a group of conditions caused by different factors but sharing similar symptoms. These include issues with the eye’s surface, tear film, or eyelids. The preocular tear film is remarkably complex, comprising a multitude of components within a carefully ordered structure. A deficiency in the quality or quantity of any one of these components can prevent the tear film from performing its important functions, resulting in ocular surface damage and dry eye symptoms. Assessment of the tear film is therefore important not only for idiopathic dry eye but also for dry eye related to systemic diseases or that induced by contact lens wear.
Resources:
2. Baudouin C, Aragona P, Van Setten G, et al. Diagnosing the severity of dry eye: a clear and practical algorithm. British Journal of Ophthalmology 2014;98:1168-1176.
3. Baudouin C, Messmer EM, Aragona P, et al. Revisiting the vicious circle of dry eye disease: a focus on the pathophysiology of meibomian gland dysfunction. British Journal of Ophthalmology 2016;100:300-306.
4. Jennifer P. Craig, Alex Muntz, Michael T.M. Wang, Doerte Luensmann, Jacqueline Tan, Sonia Trave Huarte, Ally L. Xue, Lyndon Jones, Mark D.P. Willcox, James S. Wolffsohn. Developing evidence-based guidance for the treatment of dry eye disease with artificial tear supplements: A six-month multicentre, double-masked randomised controlled trial. The Ocular Surface, Volume 20, 2021, Pages 62-69, ISSN 1542-0124, https://doi.org/10.1016/j.jtos.2020.12.006.
Novel Device for Measuring Corneal Sensitivity
The cornea, the eye’s clear front layer, is vital for vision and eye health. It is rich in sensory nerves that detect irritants and help maintain moisture [1]. Measuring corneal sensitivity objectively (by aesthesiometry) can be useful in conditions where nerve function may be altered, such as keratoconus, dry eye disease, or systemic conditions like diabetes.
To improve this measurement process, New Zealand ophthalmologist Dr Simon Dean developed a Non-Contact Corneal Aesthesiometer (NCCA), which unlike traditional methods that physically touch the eye, uses a gentle puff of air to stimulate corneal nerves, providing a more comfortable and precise approach [2]. The device delivers the air puff from a nozzle placed 1 cm from the eye, with pressure adjustable from 0.1 to 20 millibars. It also features a built-in camera for accurate alignment and a wireless remote for ease of use.
A new version of the NCCA has recently been developed to deliver cold air puffs, targeting cold-sensitive nerve fibres that may provide more detailed insight into corneal health. Researchers from The University of Auckland and The University of Melbourne, led by Professor Jennifer Craig and Dr Ceecee Britten-Jones, are studying its effectiveness compared to the original device. This novel device holds promise for advancing the research of various ocular surface diseases.

References:
1. Müller LJ, Marfurt CF, Kruse F, et al. Corneal nerves: structure, contents and function. Exp Eye Res 2003; 76: 521–542. doi:10. 1016/S0014-4835(03)00050-2
2. Swanevelder SK, Misra SL, Tyler EF, McGhee CN. Precision, agreement and utility of a contemporary non-contact corneal aesthesiometer. Clin Exp Optom. 2020 Nov;103(6):798-803. doi: 10.1111/cxo.13036. Epub 2019 Dec 23. PMID: 31869862.
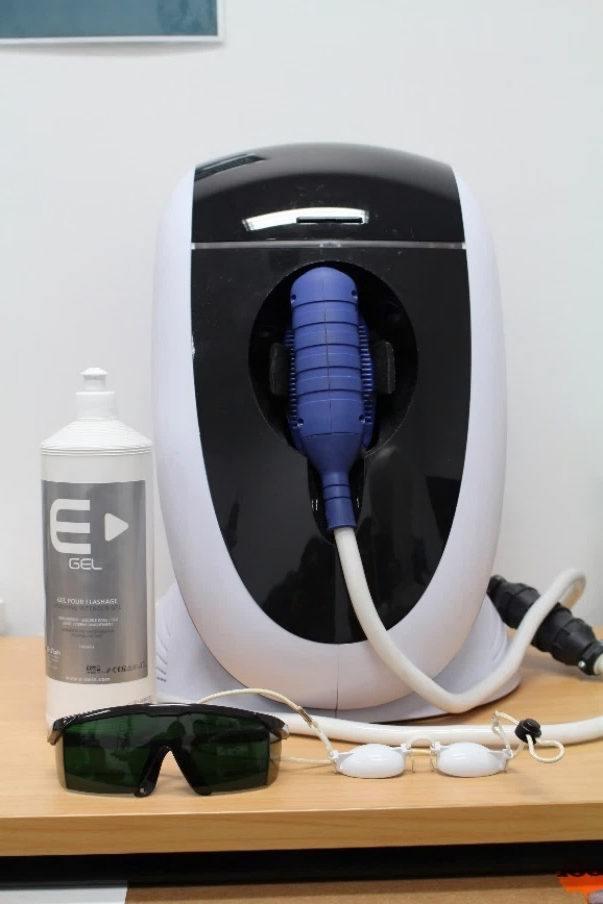
Intense Pulsed Light for Dry Eye Relief
Intense Pulsed Light (IPL) therapy is gaining recognition as an effective treatment for Meibomian Gland Dysfunction (MGD), a leading cause of evaporative dry eye disease [1]. MGD happens when the glands that produce the oil layer of tears become blocked, causing inflammation, discomfort, and tear instability. Traditional methods like warm compresses and artificial tears often offer only short-term relief, making IPL an attractive alternative [2]
A clinical trial at The University of Auckland’s Ocular Surface Laboratory explored IPL’s effectiveness in treating MGD. The study included 87 participants who were either given IPL therapy (4 or 5 light pulses) or a placebo over four months. Researchers monitored their symptoms, tear film quality, and overall eye health.
The results were promising [3]. IPL significantly improved tear stability and reduced dry eye symptoms, particularly in those who received five light pulses. Some participants noticed improvements as early as two weeks, with benefits continuing throughout the trial, including better gland function and overall eye comfort.
These findings highlight IPL as a longer-lasting, effective solution for managing MGD, offering a viable alternative to traditional treatments for those seeking sustained relief from dry eye symptoms.
References:
1. Craig JP, et al., TFOS DEWS II Report Executive Summary, The Ocular Surface (2017), ttp://dx.doi.org/10.1016/ j.jtos.2017.08.00
2. Geerling G, Tauber J, Baudouin C, et al. The International Workshop on Meibomian Gland Dysfunction: report of the Subcommittee on Management and Treatment of Meibomian Gland Dysfunction. Invest Ophthalmol Vis Sci 2011;52:2050–64
3. Xue AL, Wang MTM, Ormonde SE, Craig JP. Randomised double-masked placebo-controlled trial of the cumulative treatment efficacy profile of intense pulsed light therapy for meibomian gland dysfunction. Ocul Surf. 2020 Apr;18(2):286-297. doi: 10.1016/j.jtos.2020.01.003. Epub 2020 Jan 30. PMID: 32007523.
Clinical Assessment of Inflammation
Inflammation is a key factor in the chronic nature of dry eye disease. To address this, several topical anti-inflammatory and immunomodulatory treatments have been developed, though their effectiveness can vary, and the risks often outweigh the benefits, especially with long-term use. Identifying patients with clinically significant inflammation is essential for optimising treatment strategies.
This research project focuses on evaluating various clinical tests available to eye care practitioners for detecting increased inflammation in dry eye patients. While several tests are available, there is currently limited evidence on which is most effective for detecting increased inflammation in our patients.
Our cross-sectional clinical study gathered data on tear film and ocular surface parameters, complemented by conjunctival impression specimens analysed using droplet digital PCR to quantify known ocular surface inflammatory biomarkers. The findings from this research have been shared at both local and international conferences, and a comprehensive research paper is in preparation.

Natural Therapies for Blepharitis
Management of dry eye disease is challenging, due to its long-term nature. Ongoing effective therapeutic strategies allow patients to control their symptoms from flaring up, contributing to a better quality of life. Many patients require prolonged use of artificial tears, topical treatments and other management strategies. Consequently, there is a demand for therapies that are natural, easy to apply, cost-effective and safe to use long-term.
Natural therapies for dry eye management have been a key interest of the Ocular Surface Laboratory in recent years. Previous research includes a randomised-controlled trial investigating an eye cream featuring manuka honey, renowned for its anti-inflammatory and antibacterial properties [1]. In 2021, we became aware of the potential of castor oil as a treatment for blepharitis [2]. Following this, a paired-eye pilot study confirmed its potential in reducing the signs and symptoms of blepharitis [3].
As of 2024, we are in the process of completing a large, double-blinded, randomised, placebo-controlled study, with results expected in early 2025. We look forward to sharing our findings with the broader scientific and patient communities soon.
References:
1. Craig JP, Cruzat A, Cheung IMY, Watters GA, Wang MTM. Randomized masked trial of the clinical efficacy of MGO Manuka Honey microemulsion eye cream for the treatment of blepharitis. Ocul Surf. 2020;18(1):170-7.
2. Sandford EC, Muntz A, Craig JP. Therapeutic potential of castor oil in managing blepharitis, meibomian gland dysfunction and dry eye. Clinical and Experimental Optometry. 2021;104(3):315-22.
3. Muntz A, Sandford E, Claassen M, Curd L, Jackson AK, Watters G, et al. Randomized trial of topical periocular castor oil treatment for blepharitis. The Ocular Surface. 2021;19:145-50.
Lid-warming Treatments for Meibomian Gland Dysfunction
Meibomian gland dysfunction (MGD) is the primary cause of dry eye symptoms and can even lead to excessive tearing in some cases. In healthy eyes, meibum, the oily substance produced by meibomian glands, should be clear and easily expressed across the surface of the eyes with each blink. However, in MGD, there is reduced secretion of these oils, and their composition often becomes thickened and hardened. Effective treatment focuses on melting these hardened oils and promoting their secretion.
The current standard of care involves applying a hot compress, such as a wheat bag, to the eyelids for 10 minutes, followed by digital massage, repeated one to two times daily. Many patients find this regimen cumbersome, and adherence tends to decline when immediate relief is not experienced. To address this, in-office treatments like thermal pulsation have been developed to efficiently heat, melt and express meibum. However, these treatments can be limited in availability due to their large footprint and high costs for both practices and patients alike.
The Ocular Surface Laboratory has initiated an investigator-led research project to evaluate the effectiveness of a handheld thermal pulsation device, which offers an in-office, single treatment protocol compared to standard care methods. Results of this study indicate that this device may provide comparable outcomes, potentially serving as an effective, time-saving alternative to standard of care, over a six-month period.

Quantum Molecular Resonance for the Treatment of Dry Eye Disease
Quantum Molecular Resonance (QMR) therapy is a promising therapy for the management of dry eye disease. This therapy applies electrical currents at specific frequencies (4–64 MHz) to stimulate metabolism and natural regeneration of the cells. Studies suggest that QMR may aid in wound healing, reduce inflammation, and alleviate pain and swelling. In vitro research indicates that QMR can activate cellular pathways and promote tissue regeneration, potentially through extracellular matrix remodelling.
To address this gap, a double-masked randomized controlled trial (RCT) has been initiated to evaluate the efficacy of QMR treatment in improving the signs and symptoms of dry eye disease. This research aims to provide clearer insights into the potential of QMR as a therapeutic option for patients suffering from DED. The results have revealed encouraging outcomes that suggest that QMR is effective in treating symptoms and signs of EDE to some degree. More data specific to participants with aqueous deficiency is needed before any conclusions can be drawn about the efficacy of QMR in treating ADDE.

TFOS Dry Eye Workshops
TFOS DEWS II
In the years the Tear Film & Ocular Surface Society second Dry Eye Workshop (TFOS DEWS II) reports were published, most would agree that dry eye disease (DED) is closer to reaching household name status, becoming a disease that’s more widely recognised and acknowledged by clinicians and more readily reported by patients.
Read more
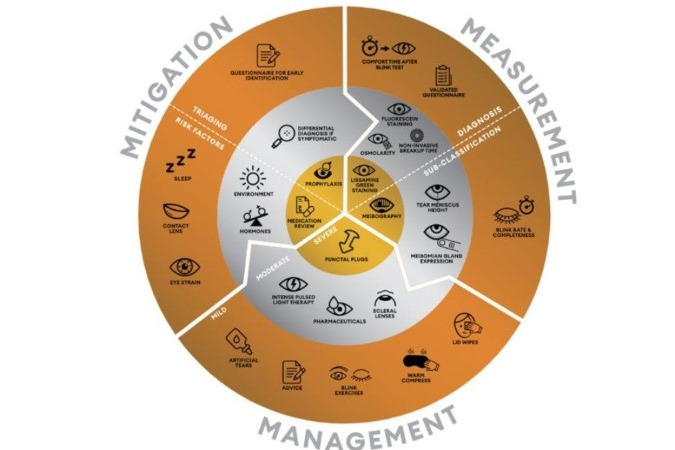
Dry Eye Assessment Algorithm
The global consensus TFOS DEWS II dry eye diagnostic test battery was developed to help provide guidance on the key outcome measures for the diagnosis and monitoring of dry eye disease in epidemiology studies and clinical trials. However, it is acknowledged that in certain resource or time-constrained settings, it might not always be feasible to conduct the diagnostic battery in its entirety, as it requires the use of several instruments and ophthalmic dyes.Read more
TFOS DEWS III
Following the success of the Tear Film & Ocular Surface’s (TFOS) second Dry Eye Workshop (DEWS II), TFOS has now unveiled details of its highly anticipated third workshop. Given the extraordinary amount of research over the past seven years, the update will focus on new and significant advances in the diagnosis, management, and classification of dry eye disease.